Professor Davis says: "These results were really unexpected. It was only possible for us to unravel the mystery of why this drug was so effective, through the use of video microscopy. By watching what happened within the cells we could clearly identify just why rituximab is such an effective drug – because it tended to reorganise the cancerous cell and make it especially prone to being killed."
He continues: "What our findings demonstrate is that this ability to polarise a cell by moving proteins within it should be taken into consideration when new antibodies are being tested as potential treatments for cancer cells. It appears that they can be up to twice as effective if they bind to a cell and reorganise it."
The findings from this study have been published online today on the website of the journal Blood. The research was carried out in collaboration with MedImmune, the global biologics research and development arm of AstraZeneca.
Commenting on the research Dr Matt Sleeman, Senior Director of Biology at MedImmune said: "Not only is this a great observation that can influence how we as a biotech company identify and design future therapies, it also shows the innovative 'out of the box' thinking that can be achieved by working in close partnership with academics at the top of their field. This unique partnership, bringing together industry and academia, demonstrates a real catalyst of scientific change within the UK, and I am excited by the potential of the MCCIR to bring further innovation that could ultimately bring benefit to patients."
Much of the research for this study was carried out during Professor Davis' time at Imperial College London. He will be continuing to use high quality video imaging at a microscopic level to investigate immunology at the MCCIR.
The Natural Killer white blood cell in red is drawn to the cancerous B cell which has been treated with rituximab. It latches on to the side of the cell where the protein CD20 (which is shown in green) has collected. The cell is then destroyed. The Natural Killer then moves on to destroy another B cell. By latching on to the side where the CD20 is gathered the NK cell has an 80% success rate in destroying the cancerous B cell.
(Photo Credit: MCCIR)

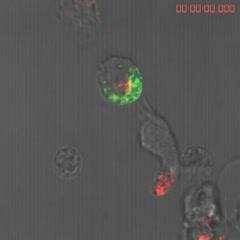
This image shows cancerous B cells that have been treated with rituximab. The protein CD20 (shown in green) has been drawn to the side of the cells. When the Natural Killer white blood cells approach they will stand an 80 percent chance of killing the cell if they latch on to the side where the protein has collected.
(Photo Credit: MCCIR)
Source: University of Manchester