Multiple sclerosis, diabetes, and arthritis are among a variety of autoimmune diseases that are aggravated when one type of white blood cell, called the immune regulatory cell, malfunctions. In humans, one cause of this malfunction is when a mutation in the FOXP3 gene disables the immune cells’ ability to function. In a new study published online this week in the Proceedings of the National Academy of Sciences, researchers at the University of Pennsylvania School of Medicine have discovered how to modify enzymes that act on the FOXP3 protein, in turn making the regulatory immune cells work better. These findings have important implications for treating autoimmune-related diseases.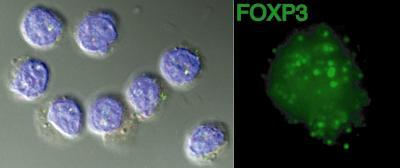 Human regulatory T cells viewed using fluorescence microscopy after immunostaining (left). FOXP3 protein stained by anti-FOXP3 antibody within one regulatory T cell (right).
Human regulatory T cells viewed using fluorescence microscopy after immunostaining (left). FOXP3 protein stained by anti-FOXP3 antibody within one regulatory T cell (right).
Credit: Kathryn T. Iacono, University of Pennsylvania School of Medicine; Proceedings of the National Academy of Sciences
"We have uncovered a mechanism by which drugs could be developed to stabilize immune regulatory cells in order to fight autoimmune diseases," says senior author Mark Greene, MD, PhD, the John Eckman Professor of Pathology and Laboratory Medicine. "There’s been little understanding about how the FOXP3 protein actually works." First author Bin Li, PhD, a research associate in the Greene lab has been working on elucidating this process since FOXP3’s discovery almost five years ago.
Li discovered that the FOXP3 protein works via a complex set of enzymes. One set of those enzymes are called histone deacetylases, or HDACs. These enzymes are linked to the FOXP3 protein in association with another set of enzymes called histone acetyl transferases that modify the FOXP3 proteins.
Li found that when the histone acetyl transferases are turned on, or when the histone deacetylases are turned off, the immune regulatory cells work better and longer. As a consequence of the action of the acetylating enzyme, the FOXP3 protein functions to turn off pathways that would lead to autoimmune diseases.
"I think this simple approach will revolutionize the treatment of autoimmune diseases in humans because we have a new set of enzymatic drug targets as opposed to the non-specific therapies we now use," says Greene. Non-specific therapies include the use of steroids and certain chemotherapy-like drugs that act on many cell types and have significant side effects.
"Before this work, FOXP3 was thought essential for regulatory T-cell function, but how FOXP3 worked was not known," says Li. "Our research identifies a critical mechanism. Based on this mechanism, treatments could be developed to modulate this regulatory cell population."
"In this line of investigation, we have learned how to turn on or off this regulatory immune cell population – which is normally needed to prevent autoimmune diseases – using drugs that are approved for other purposes, but work on these enzymes" notes co-author Sandra Saouaf, PhD, a research associate at Penn.
Li, Greene, Saouaf and Penn colleagues Wayne Hancock and Youhai Chen are now extending this research directly to several mouse models of autoimmune diseases.
Additional co-authors are Arabinda Samanta, Xiaomin Song, Kathryn T. Iacono, Kathryn Bembas, Ran Tao, Samik Basu, and James Riley, all from Penn.
Written from a news release by University of Pennsylvania School of Medicine.