February 5, 2013—Ottawa—Ottawa scientists have discovered a trigger that turns muscle stem cells into brown fat, a form of good fat that could play a critical role in the fight against obesity. The findings from Dr. Michael Rudnicki's lab, based at the Ottawa Hospital Research Institute, were published today in the prestigious journal Cell Metabolism.
"This discovery significantly advances our ability to harness this good fat in the battle against bad fat and all the associated health risks that come with being overweight and obese," says Dr. Rudnicki, a senior scientist and director for the Regenerative Medicine Program and Sprott Centre for Stem Cell Research at the Ottawa Hospital Research Institute. He is also a Canada Research Chair in Molecular Genetics and professor in the Faculty of Medicine at the University of Ottawa.
Globally, obesity is the fifth leading risk for death, with an estimated 2.8 million people dying every year from the effects of being overweight or obese, according to the World Health Organization. The Public Health Agency of Canada estimates that 25% of Canadian adults are obese.
In 2007, Dr. Rudnicki led a team that was the first to prove the existence of adult skeletal muscle stem cells. In the paper published today, Dr. Rudnicki now shows (again for the first time) that these adult muscle stem cells not only have the ability to produce muscle fibres, but also to become brown fat. Brown fat is an energy-burning tissue that is important to the body's ability to keep warm and regulate temperature. In addition, more brown fat is associated with less obesity.
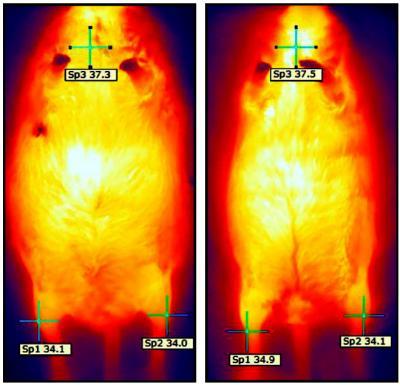
In this picture taken with a thermographic camera after four months, the mouse treated with miR-133 ASO (on the right) is noticeably leaner. In addition, the injected hind leg (on the left in the image) is 0.8 C hotter than the control mouse.
(Photo Credit: Rudnicki et al., Ottawa Hospital Research Institute, published in Cell Metabolism)
Perhaps more importantly, the paper identifies how adult muscle stem cells become brown fat. The key is a small gene regulator called microRNA-133, or miR-133. When miR-133 is present, the stem cells turn into muscle fibre; when reduced, the stem cells become brown fat.
Dr. Rudnicki's lab showed that adult mice injected with an agent to reduce miR-133, called an antisense oligonucleotide or ASO, produced more brown fat, were protected from obesity and had an improved ability to process glucose. In addition, the local injection into the hind leg muscle led to increased energy production throughout the body—an effect observed after four months.
Using an ASO to treat disease by reducing the levels of specific microRNAs is a method that is already in human clinical trials. However, a potential treatment using miR-133 to combat obesity is still years away.
"While we are very excited by this breakthrough, we acknowledge that it's a first step," says Dr. Rudnicki. "There are still many questions to be answered, such as: Will it help adults who are already obese to lose weight? How should it be administered? How long do the effects last? Are there adverse effects we have not observed yet?"
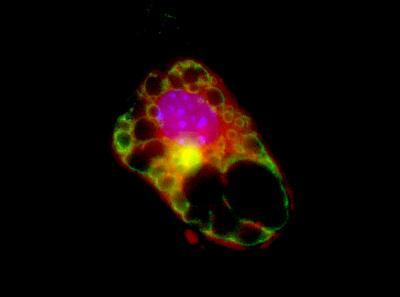
This is a photomicrograph of a brown fat cell (brown adipocyte) derived from a muscle stem cell that was induced by using an agent to reduce the amount of miR-133.
(Photo Credit: Alessandra Pasut, Ottawa Hospital Research Institute)