The presence of specific autoantibodies of the immune system is associated with blood vessel damage in the brain. These findings were made by Marion Bimmler, a graduate engineer of medical laboratory diagnostics at the Max Delbrück Center for Molecular Medicine Berlin-Buch and Dr. Peter Karczewski of the biotech company E.R.D.E.-AAK-Diagnostik GmbH in studies on a rat model. The researchers' results suggest that autoimmune mechanisms play a significant role in the pathogenesis and progression of Alzheimer's and vascular dementia (PloS ONE, doi:10.1371/journal.pone.0041602)*.
Antibodies are the defense molecules of the body's immune system against foreign invaders. If the antibodies cease to distinguish between "foreign" and "self", they attack the cells of the own body, and are thus referred to as autoantibodies. These can trigger autoimmune diseases. Using MR angiography and other methods, Marion Bimmler and her colleagues have now shown that the autoantibodies bind to specific surface proteins (alpha1 andrenergic receptors) of vascular cells and thereby damage the blood vessels of the brain. The reason: The autoantibodies generate a continual stimulation of the receptor and at the same time trigger an increase in intracellular calcium ion levels. As a result, the blood vessel walls thicken, and blood flow to the brain is disturbed.
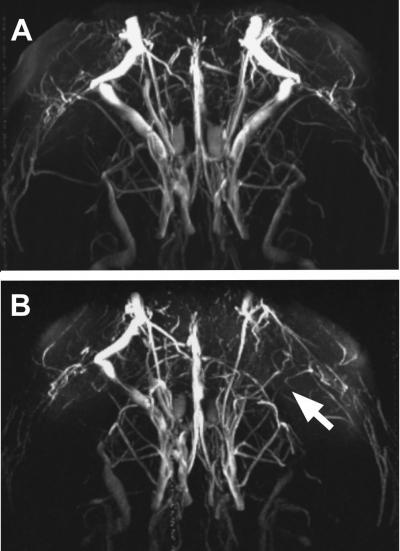
The presence of specific autoantibodies of the immune system is associated with blood vessel damage in the brain. These findings were made by by Marion Bimmler, a graduate engineer of medical laboratory diagnostics at the Max Delbrück Center for Molecular Medicine Berlin-Buch and Dr. Peter Karczewski of the biotech company E.R.D.E.-AAK-Diagnostik GmbH in studies on a rat model. Their results suggest that autoimmune mechanisms play a significant role in the pathogenesis and progression of Alzheimers and vascular dementia. The MR Angiography shows that antibodies damage blood vessels in the brain of rats (see arrow in image B). Eight months after the rats were administered an antibody against a surface protein (alpha1-adrenergic receptor) in the vascular cells, the blood vessels are hardly recognizable, because the blood flow has been interrupted. Image A shows the blood vessels (white) in the brain of healthy animals with no antibodies. These findings are important for understanding the pathogenesis and progression of Alzheimers disease and vascular dementia.
(Photo Credit: (MR Angiography/Copyright: MDC))
First Encouraging Results after Removal of Autoantibodies by Immunoadsorption
In earlier studies, Marion Bimmler and her research team examined blood samples of patients with Alzheimer's or vascular dementia and showed that half of them had comparable autoantibodies. A first clinical trial together with Charité – Universitätsmedizin Berlin is currently ongoing with a collective of patients with Alzheimer's or vascular dementia. The patients were divided into two groups – a small group whose autoantibodies were removed from the blood via immunoadsorption and a control group that did not receive this treatment. Until now, over an observation period of 6 and subsequently 12 months, the patient group who had undergone immunoadsorption improved in their memory performance and in their ability to cope with their everyday lives. In contrast, the condition of the patients who did not receive immunoadsorption treatment and continued to have autoantibodies in their blood deteriorated dramatically. Now the researchers are planning further clinical trials with larger numbers of patients.